By Parson Rambinizandry (Velondriake Safidy Programme Coordinator) & Marie Williamson (Safidy Medical Officer)
Two months ago we sat down with some of our community health workers to brainstorm ideas for International Women’s Day. What would engage women, what could bring about positive change in their community? Something different to the normal celebrations, perhaps a petition for a midwife? This seemed like a great idea on paper, but would it create false hope in a village where the public health centre has been closed for years?

Women in Andavadoaka sign the community petition for a midwife.
In Madagascar, the chance of dying from pregnancy-related complications remains high; Malagasy women face a 1 in 43 lifetime risk of maternal death. This national statistic masks an even tougher reality in rural settings where healthcare facilities are few and far between, and where travel is difficult; often uncomfortable for pregnant women and can mean forgoing livelihoods. Most women deliver at home, with or without a traditional birth attendant, although many would prefer to deliver in a health centre with a skilled midwife or nurse.
Behind each number there is a woman and a baby, a family and a community. To illustrate these numbers, here are a couple of stories from the time when we provided antenatal care in the absence of a government midwife…
A 32 year-old lady from a remote island presents in her tenth pregnancy. Three of her children have died. She is at greater risk of bleeding during the delivery because of the number of babies that she has had. She will probably deliver at home without medication to prevent bleeding after the delivery of her baby; she has little other choice.
A 14 year-old girl attends in her second term of pregnancy. It is not unusual to see girls at this age falling pregnant. This girl is at high risk of complications during labour and delivery due to her young age. On top of this, she will no longer be able to complete her education locally, even after her baby is born, due to the school rules.

Havany, aged 24 years, gave birth to a healthy baby boy a few weeks ago. Like the majority of women in her village, she delivered at home without the assistance of a trained midwife. Luckily she experienced no complications, but others are not so fortunate. Photo © Garth Cripps for Blue Ventures.
Following some devastating newborn deaths in the village of Andalambezo, near Andavadoaka, their community health worker felt moved to mobilise women to take action, and we recently supported the creation of a women’s group in this village. Two questions were asked at the first session: do you know someone who has died in pregnancy/delivery, and do you know a baby who has died at a very young age? Sadly, all hands went up for both of these questions. This served as a reminder of how desperate the situation can be in rural Madagascar. Of the nine women who had given birth since January, four ended in a stillbirth.
Trained midwives are essential for improving these adverse outcomes. They offer antenatal care including regular monitoring, anti-tetanus vaccinations, STI testing and treatment, folic acid and iron tablets, and presumptive treatment of malaria and intestinal worms. They provide skilled facility-based delivery and postnatal care, including breastfeeding advice and childhood vaccinations. But it seemed like a pipe dream for a government midwife to be placed in Andavadoaka…
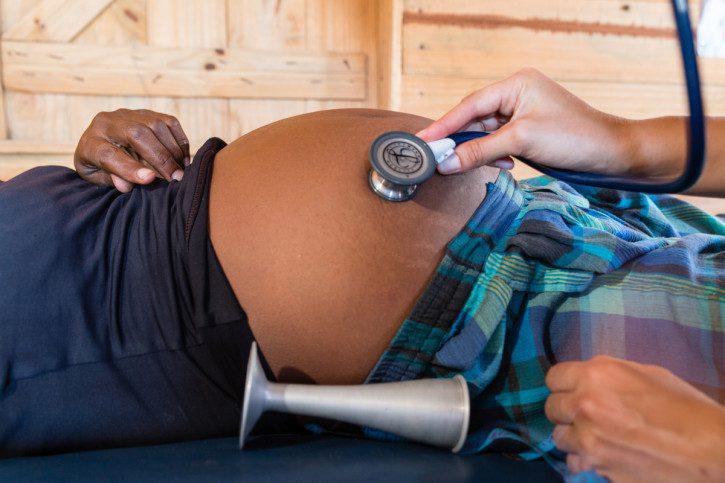
Photo © Garth Cripps for Blue Ventures.
Our first petition – written by local women, signed by 155 people and stamped with a local seal of approval – was presented to the district medical inspector, who congratulated the community for their initiative. Unfortunately though, no government healthcare post would be possible in Andavadoaka for the foreseeable future, as the Ministry of Health had already decided to reopen the public health centre in Befandefa (the commune centre). There’s no easy way for pregnant women from the surrounding area to travel to Befandefa without walking for hours or taking an uncomfortable and expensive zebu cart, so we persisted in our advocacy efforts.
Parson, coordinator of our Safidy community health programme, engaged in meetings with the regional health director, presenting the petition (now with almost 200 signatories) and explaining the situation in Andavadoaka. Acknowledging the Ministry of Health’s strong collaborative relationship with Blue Ventures and praising our work to empower women to bring about positive change in their own community, the regional health director responded to this request by agreeing to prioritise reopening a government healthcare post in Andavadoaka.

More photos here!
The timing could not have been better! At the end of March, the Ministry of Health announced they would be (re)opening 100 health centres in 100 days. Caroline, our national Population-Health-Environment coordinator, met with Ministry of Health officials in the capital of Antananarivo, while Parson held further meetings with the regional health director and the district medical inspector.
Before long, our petition had transformed from photos and signatures into reality and formalities. We couldn’t quite believe that it was a yes!

A few weeks later, we welcome Christina – the new government midwife – to Andavadoaka with a joyful inauguration ceremony! She’s enthusiastic and promises to diligently serve the community of Andavadoaka, especially the women who have campaigned for her to be placed here. Healthcare professionals from across the region are in attendance, including the new nurse for Befandefa who had been installed the previous day.
Speeches are made by the district medical inspector, the adj. mayor of Befandefa, and the president of the Velondriake locally managed marine area association. They all reiterate how instrumental the local women have been in bringing Christina to Andavadoaka, by demonstrating their motivation to have a midwife and audaciously standing up for this issue that affects the health of their community.
What a feat for these ladies! Many had not imagined the power of their own voice or signature. We hope that this achievement will give them confidence and encouragement to campaign for more change about other issues that matter to them.

Christina, at her welcome ceremony!
And so our Safidy centre has been rapidly converted into a temporary public health centre, while the government constructs a purpose-made building from which Christina can serve. She’s now in charge of providing antenatal and postnatal clinics, mother and child vaccinations, and of course assisting with deliveries! In addition to her clinical role, we’re excited that she’s agreed to facilitate training sessions for our community health workers and partner with them on improving community health overall.
Asking women about their proposed place of delivery always used to bring the same answer; “At home with a traditional birth attendant, without any other choice”. Often we wondered why we asked. Happily this has changed now, and for the first time the reply comes with a smile; “I’ll deliver here, with the midwife.” Tonga soa, Christina!
Blue Ventures would like to thank the Madagascar Ministry of Health, regional health director and district medical inspector for their valuable collaboration and support.

