When I talk to new mothers in the communities we work with, most say “I gave birth with the mpagnavagnavana.”
Mpagnavagnavana is the Malagasy word for traditional birth attendants (TBAs), but literally translates to “mother of the child”. This accurately reflects the significance of their role, they help give life to children and are considered as mothers by their communities.
Women in these communities will often actively prioritise TBAs over other forms of maternal health provision, trusting in their advice and experience.
Blue Ventures’ community health team in the Ambanja district of northwest Madagascar recently completed a community diagnostic survey to identify health needs across 12 villages. This survey highlighted that TBAs are a crucial resource for pregnant women, particular in rural areas with poor access to health centres and low levels of income. Women in these communities will often actively prioritise TBAs over other forms of maternal health provision, trusting in their advice and experience.
The survey also clarified the extent of the role that TBAs play. They advise women during their pregnancies, deliver children in the mother’s home and provide postnatal consultations. In short, TBAs do very similar work to the healthcare professionals based in government health centres, and yet there is very little collaboration. The survey found that the TBAs around Ambanja only work with community health workers and government health workers in the case of complications, even if these health workers are present in the village. Despite the average TBA delivering three to four children per month, hardly any have been involved in formal birth registrations.
Community meetings were held in each surveyed village, and the TBAs were very open about their practices. We learnt that their work is based on many generations of experience, often within the same family from grandmothers and great grandmothers.
“We always use the kosombolo [a simple razor] or scissors to cut the umbilical cord, and we recommend herbal teas for pregnant women in their first trimester, sometimes even before conception.”
We also learnt that some TBAs were in need of more or better resources, with several communities voicing that “the mpagnavagnavana need more equipment and a place for them to deliver children in the village.”
With our new awareness of exactly how vital TBAs are for maternal and child health in these communities, and their unmet need for training and resources, we started working on ways to bring TBAs and health workers together.
The first stage in this plan was to meet with the Medical Inspector of Ambanja, to report our findings from the survey and community meetings, and discuss potential collaboration activities with TBAs. The Medical Inspector agreed that there was a need for collaboration, and more meetings were held with the district’s health centres to clarify goals and responsibilities.
However for TBAs to collaborate with government health centres, they also needed to conform to international health regulations, and approval was needed from Madagascar’s Ministry of Health. It took ten months before everything was finally in place and, in partnership with the Ministry of Health, we were able to organise an information and exchange session for the 18 TBAs in the Ambanja area.

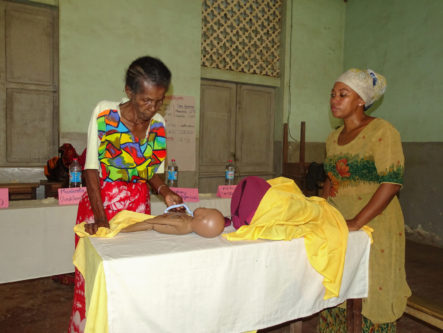
The information and sharing session for health workers and TBAs | Photo: François Rakotoarisoa
Two hours before the beginning of the session, two of the TBAs had already arrived! Both of them showed me their invitations, and then one of them said “we didn’t want to be late and miss the beginning of the training. We are really interested in improving our traditional practices.” By the time the training began, 14 of the 18 TBAs were present. An encouraging attendance for such a new initiative.
During the session the TBAs continued to express their motivation to learn, and freely shared their personal experiences of delivering babies. Only one of them had previously collaborated with health workers, describing how she had accompanied women to health centres and used gloves there to prevent infections. The rest had never visited the health centres except as a last resort in a birth with serious complications.
“During the prenatal visits we know beforehand if a woman is likely to have complications and then we refer them to a health centre,” stated one the TBAs, adding “regardless, some women will still just go to another mpagnavagnavana rather than a health centre.”
Taking into account the TBAs’ testimonies about the reality of life in their villages, an overview was given of the differences between their services and the services offered at health centres, highlighting areas where collaboration would be beneficial.
It was agreed that TBAs should ask their clients to attend pre and postnatal consultation sessions at health centres to ensure that the babies receive their birth certificates and the appropriate immunisations, that health workers and TBAs in the same community should collaborate in promoting best practices for maternal and newborn health, and that TBAs should refer women and children to health centres when screening for specific diseases.
In their closing speech at the end of the session, the Medical Inspectors said “I hope and trust that these collaborations will help reduce the child mortality rate in the Ambanja district.”

The TBAs and health workers after the session | Photo: François Rakotoarisoa
12 days later, we followed up with the TBAs and discovered that one had accurately diagnosed a woman with a condition discussed during the session, 13 women had been referred to health centres for prenatal consultations and three for postnatal consultations, and that one of the TBAs had bought themselves ten pairs of sterile gloves.
These early results suggest that the TBAs are serious in their desire to improve their practices and increase collaboration, and they demonstrate just how often they are called upon to serve their communities.
We hope to continue seeing the benefits from the information and exchange session during our weekly visits to the TBAs, and another session will be hosted in three months’ time to evaluate the progress and assess more potential collaboration opportunities.
The national community health policy in Madagascar states that the effectiveness of community health is determined by the awareness, involvement, empowerment, and active participation of the community. As influential members of their communities, increased collaboration between TBAs and health centres will help transmit key health messages, increase community engagement and increase overall community health in the Ambanja district and other remote areas of Madagascar.
Thanks to the Helmsley Charitable Trust, the MacArthur Foundation, and all supporters of our community health programme
Discover why Blue Ventures started supporting community health in Madagascar